Views: 222 Author: Edvo Publish Time: 2025-12-21 Origin: Site











Content Menu
● Understanding the Basics: Orthotics vs. Insoles
● The Core Issue: Can You Layer Them Together?
● Why Wearing Orthotics over Insoles Can Be Problematic
>> 1. Instability and Misalignment
>> 4. Premature Wear and Friction
● When Layering Orthotics and Insoles Works
>> 1. Temporary Cushioning for Adaptation
>> 2. Shoes with Deep or Spacious Interiors
>> 3. Lightweight Comfort Liners
>> 4. Special Occupational Needs
● How to Properly Fit Custom Orthotics into Shoes
● Adapting to New Orthotics: What to Expect
● Choosing Orthotic-Friendly Footwear
● Signs You're Wearing Orthotics Incorrectly
● Maintenance and Longevity Tips
● Extra Comfort Techniques for Orthotic Users
● Importance of Professional Guidance
● FAQ about Wearing Orthotics over Insoles
>> 1. Can I wear orthotics and insoles at the same time?
>> 2. Should I remove the shoe's factory insole before adding orthotics?
>> 3. Is there any situation where using both is beneficial?
>> 4. How can I tell if my orthotics are not fitting properly?
>> 5. How often should I replace my custom orthotics?
For anyone who struggles with foot pain, instability, or daily fatigue, orthotic insole often seem like essential tools. Both aim to improve the way your feet interact with the ground, offering relief, stability, and better posture. However, many people ask the same question when trying to get the best of both worlds: Can you wear custom orthotics over insoles?
This question may sound simple, but the answer depends on several factors — including the design of your shoes, the purpose of your orthotics, and how your feet respond to additional cushioning. By exploring these factors in depth, you can make an informed decision that enhances comfort while maintaining proper biomechanical function.
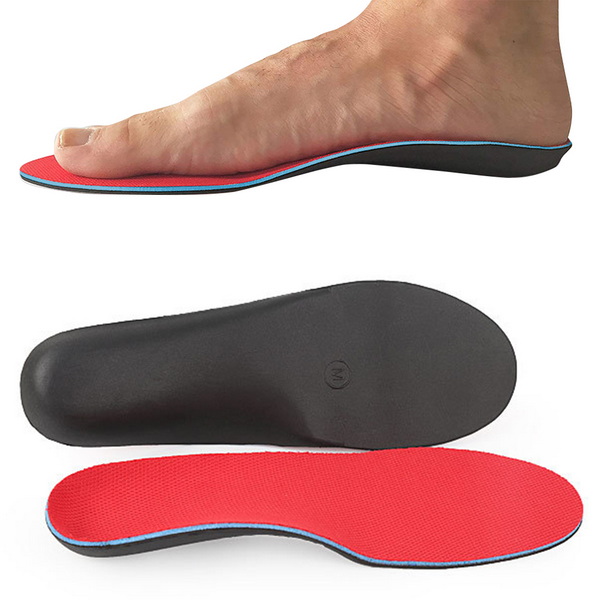
Many people confuse orthotics and insoles, but they actually serve very different purposes. Knowing how each works helps explain why layering them isn't always beneficial.
Custom orthotics are medical-grade foot devices designed to correct specific foot and posture issues. They are typically prescribed by podiatrists after a professional assessment or digital foot scan. Every orthotic is precision-crafted based on your unique foot shape, pressure distribution, and gait pattern.
The main goals of custom orthotics include:
- Correcting misalignments such as overpronation or flat feet.
- Reducing pain in common problem areas like the heel, arch, or ball of the foot.
- Supporting the kinetic chain from feet to knees, hips, and spine.
- Improving efficiency during movement for athletes and active users.
Custom orthotics come in different styles depending on your needs—rigid, semi-rigid, or accommodative. Rigid orthotics control motion; semi-rigid ones balance support and flexibility; and accommodative versions focus on cushioning sensitive pressure areas, ideal for conditions like diabetic foot or arthritis.
In contrast, insoles are removable shoe inserts made for general comfort. They typically come pre-installed in your footwear but can be replaced or upgraded. Unlike orthotics, insoles are not designed to correct medical issues. Instead, they enhance comfort, absorb shock, control moisture, or add extra cushioning for long wear.
Common insole types include:
- Foam insoles: Light and cushy, suitable for daily comfort.
- Gel insoles: Excellent for shock absorption and pressure relief.
- Memory foam insoles: Molds to your foot's shape for a custom feel.
- Special-purpose insoles: Designed for odor control, warmth, or cooling.
Insoles improve comfort but do not offer precise biomechanical correction. That's why they're often used in everyday footwear, while orthotics target deeper structural or medical needs.
Whether you can wear custom orthotics over insoles depends on your shoe type and the intended function of each insert.
Generally, it is not recommended to place custom orthotics on top of insoles, especially thick or contoured ones. Orthotics require a firm and stable surface to maintain correct positioning and alignment. If you put them over a soft or uneven base, they may tilt, compress, or move out of place, making them less effective and even uncomfortable.
However, not all shoes and users are the same. There are exceptions where using both can work — but only when done carefully and with attention to fit.
Stacking orthotics and insoles inside the same shoe introduces several biomechanical and comfort challenges.
Orthotics need a stable foundation to guide the foot's natural movement. When placed on top of a soft or shaped insole, their base can shift with pressure. As a result, your feet may land unevenly, altering gait patterns and causing new pressure points rather than relieving existing ones.
Most shoes are made with specific internal volume. Adding extra layers reduces this space, compressing your toes and midfoot. This tightness can lead to blisters, numbness, or circulation problems. It can also tilt your heel higher inside the shoe, disturbing ankle alignment and overall comfort.
Since custom orthotics are made from precision measurements, even a few millimeters of height difference can affect their purpose. This may compromise the orthotic's corrective potential, effectively wasting the benefits you invested in.
Two layers rubbing against each other cause friction, leading to faster deterioration of both inserts. Over time, edges may peel or curl, making the orthotic unstable or unusable.
Although generally discouraged, there are specific situations where combining orthotics and insoles can be appropriate and even beneficial.
People new to orthotics often experience mild soreness as their feet adjust. In the first week or two, placing a thin insole or liner beneath the orthotic can make the transition smoother. Once your body adjusts, you can remove the extra layer.
Some shoes—particularly orthopedic or sport models—come with deeper footbeds or removable insoles specifically designed for orthotic use. In these cases, you may place a thin cushioning layer under the orthotic without overcrowding the shoe.
If your orthotic feels too rigid for daily wear, a 1–2 mm thin comfort liner may add softness while preserving biomechanical accuracy. The key is to avoid thick insoles that raise your heel or alter alignment.
Workers in high-impact or long-hour environments, such as warehouse staff, nurses, or retail employees, may benefit from mild cushioning beneath their orthotics to lessen fatigue while still maintaining corrective support.

When using orthotics—alone or with a liner—fit is everything. Follow these steps for the best outcome:
1. Remove the original insole: This ensures sufficient space and a stable base for the orthotic.
2. Check depth and width: The shoe should have enough room to accommodate the orthotic without squeezing your foot.
3. Position carefully: The orthotic must sit flat and reach the same length as the shoe's original insole. Any shortening or curling can affect comfort.
4. Test gradually: Wear them for one or two hours per day initially, then slowly increase wear time to allow your feet to adapt.
5. Observe alignment: Standing naturally, ensure your heel rests securely in the cup and your arch aligns without pressure or pain.
If your shoes feel too tight or unstable, avoid forcing the fit. A professional adjustment or slightly larger shoe size may be necessary.
It's normal to feel some tightness, pressure, or mild discomfort during the break-in period for custom orthotics. Your muscles and joints are adjusting to improved posture and alignment.
During this adaptation period:
- Alternate wear time between your orthotic shoes and normal shoes.
- Check for any signs of redness or soreness on your feet.
- Ask your podiatrist for follow-up adjustments if discomfort persists beyond two weeks.
Proper adjustment ensures that orthotics not only improve comfort but also retrain your body mechanics for long-term stability.
Your shoes play a major role in how effective your orthotics are. The best footwear for orthotics typically features:
- Removable insoles: Allowing direct placement of custom orthotics.
- Firm heel counters: Keeping your heel stable.
- Supportive midsoles: Providing structure under the orthotic.
- Deep interiors: Preventing crowding after inserting orthotics.
- Lace-up or adjustable closures: Securing a snug but comfortable fit.
Running shoes, hiking boots, and orthopedic models often meet these criteria. If you wear dress or fashion shoes, consider special slim orthotics made for tighter spaces.
Incorrect usage or layering can lead to more problems than solutions. Watch out for these warning signs:
- Persistent foot pain or new discomfort in the knees or back.
- Tingling or numbness after a short period of use.
- Uneven shoe wear patterns.
- Visible gaps or movement under the orthotic.
If you experience any of these issues, revisit your fitting or consult your orthopedic specialist. Correct alignment should relieve pain—not create it.
Both orthotics and insoles wear out over time. Proper care helps you extend their lifespan and maintain performance.
- Clean regularly: Wipe orthotics with a damp cloth and mild soap. Let them air dry naturally.
- Avoid moisture accumulation: Remove them after extended use to let the shoes and inserts dry.
- Replace if warped or cracked: Once the structure changes, support decreases.
- Store them flat: Keep orthotics in a cool, dry place to prevent deformation.
Most custom orthotics last between two to five years depending on material quality, body weight, and usage pattern. Periodic checkups ensure you continue to receive appropriate support.
For those who still seek additional comfort even with orthotics, there are alternative methods besides layering full insoles:
- Cushioning socks: High-quality padded socks reduce friction and pressure without disrupting orthotic alignment.
- Heel pads or metatarsal supports: Use selectively under the orthotic for targeted comfort.
- Dual-density footwear: Shoes with built-in cushioning midsoles often eliminate the need for extra insoles.
- Custom orthotic covers: Some specialists can apply softer surface materials to your orthotic top layer for enhanced feel.
Small, strategic adjustments like these are safer and more effective than double-layer inserts.
Self-adjusting your shoe inserts can sometimes do more harm than good. If you are unsure whether your shoes allow layering or if you need additional comfort support, seek help from professionals such as podiatrists or certified orthotic technicians.
They can evaluate your foot pressure distribution and recommend whether a thin liner or insole addition is appropriate. They might also adjust the orthotic's thickness or curvature to restore balance if your shoes vary in depth or shape.
Remember: comfort should never come at the expense of posture or support integrity.
Wearing custom orthotics over insoles may seem tempting for a softer feel, but generally, it is not recommended. Orthotics function best when positioned directly on a firm, flat base—allowing them to guide your feet correctly. Adding extra layers can interfere with alignment, stability, and shoe fit.
If you need added cushioning, consider thin liners, orthotic-friendly shoes, or padded socks instead of full insoles. Always consult your healthcare provider before combining inserts, especially if your orthotics are prescribed for medical reasons.
Properly fitted orthotics can transform the way you walk, stand, and move—helping you enjoy better comfort, posture, and foot health without compromise.

In most cases, no. Orthotics are medical devices that need a stable surface to work effectively. Layering thick insoles underneath may alter alignment and reduce support precision.
Yes. Always remove the original insole to create room for your orthotics. This ensures a more natural fit and prevents overcrowding inside the shoe.
It can be acceptable during a short adjustment period or when the added layer is extremely thin, such as a low-profile comfort liner designed to reduce friction.
If you feel pressure points, numbness, or instability after wearing them for several days, they may not be aligned correctly or the shoe may lack adequate space.
Every two to five years, depending on daily wear, material type, and mobility level. Visiting your podiatrist annually ensures your orthotics are still suitable for your needs.
Open-Cell vs Closed-Cell EVA Inserts: Which Offers Better Moisture Management in Tropical Climates?
Carbon Fiber Insoles vs Rebound Foam: Balancing Rigidity and Cushioning in High-Impact Basketball
Memory Foam vs PU Footbeds: Which Material Actually Prevents Standing Fatigue for 12+ Hour Shifts?
PU vs EVA Foam Insoles: A Long-Term Durability Test for Industrial Work Boots
A Step-by-Step Expert Guide to Replacing Your Shoe Insoles (With OEM Insider Tips)